Women who were able to opt for NIP often said that they were very satisfied of their choice and felt that they were well-informed. There is however still a need to examine how women get access and comprehend information regarding NIPT and the way they are provided with counsel during pregnancy to make informed and independent decisions.
Non Invasive Prenatal Testing and Reproductive Planning
In the future, as NIPT becomes more widely available as it becomes more accessible, it is essential that clinicians are knowledgeable on how to provide accurate and clear details about the test. Qualitative research has shown that women desire and require access to top-quality information concerning NIPT in order to take their own decisions. This is essential for increasing reproductive autonomy, which is among the fundamental values of informed choice.
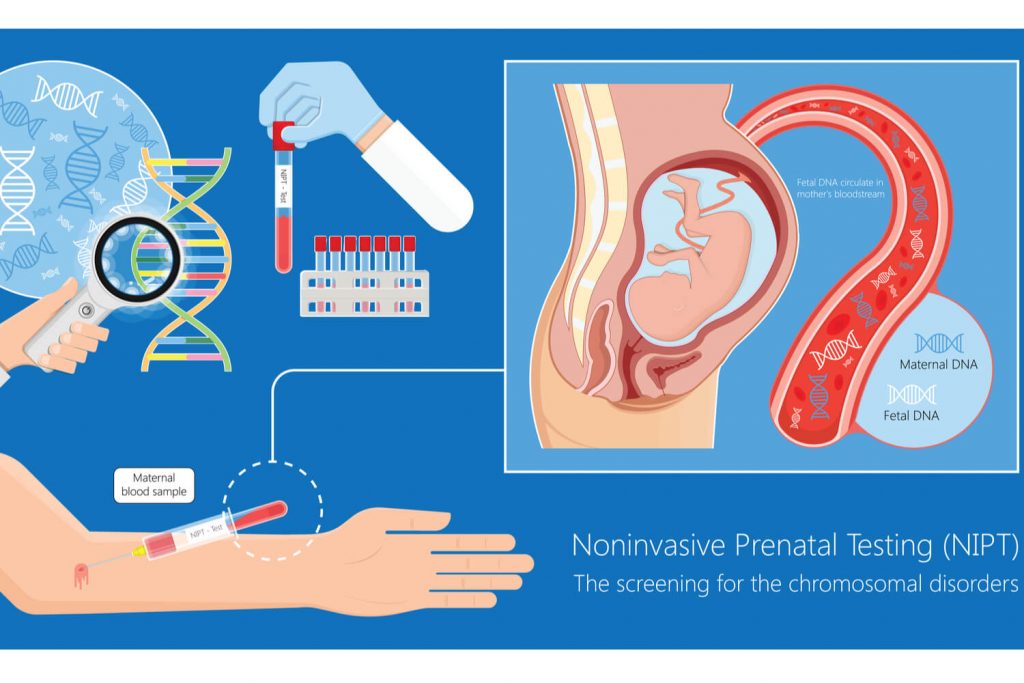
The test NIPT is a non-invasive one which uses a small amount of mother’s blood in order to identify the presence of chromosomal disorders within her child. It can detect Edward syndrome (duplication of the X and Y chromosomes), Patau syndrome (trisomy 13), and Down syndrome (trisomy 21). If positive results are found, an additional diagnostic test, such as amniocentesis, or CVS could be required to verify the result.
Genetic Abnormality Detection in Reproductive Planning
NIPT doesn’t pose any risks to women who are pregnant, as opposed to test for diagnosing such as amniocentesis as well as chronic villus sample (CVS). It utilizes cell-free DNA (cfDNA) taken from the mother’s blood sample to determine aneuploidy by counting chromosomes.
The test is a good choice for pregnancies with high risks as well as those who are not a good candidate for surgery that is invasive. But, the results may not be 100% accurate.
They also emphasized that, If NIPT gets standardized and made available as a normal prenatal test can hinder reproductive autonomy and increasing the likelihood of social stigma towards people disabled and cause inappropriate use of the tests. To prevent this professional experts emphasized that the counselling must not just explain the technical details of NIPT and correct misunderstandings about disability and testing, but also explore women’s attitudes to NIPT, and the intention to have children with disabilities.
Role of NIPT in Family Planning
It is a screening test but is not a diagnostic instrument. If results from NIPT suggest a risky presence of the presence of an anomaly, her OB/GYN or midwife could suggest more invasive diagnostic genetic tests, such as chorionic villus sample (CVS) and amniocentesis. They involve taking a tiny amount of placenta from the uterus, with a small possibility of miscarriage.
A few respondents believed that the screening for pre-tests in NIPT xet nghiem nipt ha noi vietgen must be redesigned as it’s crucial to women having access to this information, however they’re not always able to be able to make educated decisions based on the details given. The expansion of the NIPT scope to encompass more types of conditions could have to incur more cost out-of-pocket, that could be disproportionately affecting low-income women.
Respondents were also concerned they NIPT may result in the birth of children with Down syndrome as well as Edwards Patau’s syndrome or ‘- syndrome. They believed this would increase the costs of caring for the children in addition to their requirement for support and special education services.
Ethical Considerations in Prenatal Decision Making
There are ethical concerns when women are offered NIPT in public health systems. The participants in our study are generally against the idea of a policy which would prioritise accessibility to NIPT for certain conditions as they believed that the determination of whether reproductive outcomes are ‘worth living in the discretion of couples and not be based on priori appraisal of how serious each condition is.
The blood of a pregnant woman is a reservoir of DNA and sperm from her fetus, known as fetal cell-free DNA (cffDNA). The NIPT test analyses this cffDNA for the purpose of determining whether there is or absence of particular genetic disorders like Down syndrome as well as other chromosomal disorders. The participants were worried that the testing process could give the impression of pressure to test, because of concerns regarding industry influence in educational materials and incentives to health professionals to encourage the NIPT.
Access and Cost of NIPT in Reproductive Planning
NIPT costs more than most tests for screening and is not covered by Medicare or private health insurance in Australia. It is suggested that women consider their options with a genetic counsellor before deciding whether to take the test.
The DNA of a growing baby is present throughout the mother’s bloodstream. scientists can detect it using an easy laboratory test. It is referred to as the cell-free fetal DNA (cffDNA). NIPT requires only a small sample of maternal blood, and does not place the mother at threat.
The qualitative interview with women who were interviewed by Van der Meij and colleagues reveal that the majority of women who opted for NIPT did so because it gave them reassurance and additional knowledge about their pregnancy. However, many women who refused the test did it as they believed that there was no moral obligation to undertake it.